Exceptional treatment
for glaucoma at our clinic
Glaucoma is a disease that damages your eye’s optic nerve. The optic nerve is like the cable that connects the eye to the brain. When the optic nerve is damaged, visual input from the eye is prevented from being properly transmitted to the brain for interpretation.
When fluid builds up in the front part of your eye, it increases the pressure on your eyes and damages the optic nerve. It’s a leading cause of blindness for people who are over 60 years, and is the leading cause of irreversible blindness worldwide. Glaucoma affects about 4% of Americans.
Glaucoma runs in families, and is more common in certain racial and ethnic groups.

Visit us today for your glaucoma treatment!
Dr. Thayer is a fellow of the American Academy of Ophthalmology and is fully board certified by the American Board of Ophthalmology.
Major Types of Gluacoma
examining the differences

Primary open-angle glaucoma – The eye doesn’t drain fluid properly, which damages the optic nerve due to the pressure within the eye. Some people have optic nerves that are sensitive to normal eye pressure, making them vulnerable to glaucoma. As this type of glaucoma is painless and doesn’t result in vision loss in early stages, it can only be detected through regular eye checkups.

Angle-closure glaucoma – Also known as “closed-angle glaucoma” or “narrow-angle glaucoma,” this glaucoma occurs when the iris is too close to the drainage angle in the eye. The iris could block the drainage angle, increasing the eye pressure quickly. This is called an acute attack and needs to be treated immediately. Some symptoms of acute angle-closure glaucoma attack are blurry vision, severe eye pain, headache, nausea, vomiting, and seeing rainbow-colored rings or halos around lights
Diagnosing Glaucoma
factors and procedures
Glaucoma diagnosis consists of:
- Family History
- Measurement of intraocular pressure (IOP)
- Assessment of the optic nerve
- Visual appearance
- Ocular Coherence Tomography
- Visual Field
- Assessment of Corneal Thickness
- Gonioscopy
- Occasionally, CT or MRI of the eye socket and brain
With the exception of the CT or MRI, we perform all of these tests right in the office at Westfield Eye Center.
Not uncommonly, diagnosing glaucoma may take several visits over months, even years. Patients undergoing such long term evaluation are known as glaucoma suspects, as they will have one or more risk factors or signs suggestive of glaucoma, but do not have enough of them to actually make a definitive diagnosis.
diagnostic tools include
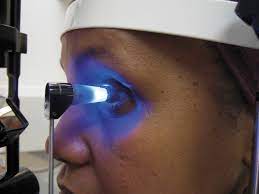 Eye pressure is the most important risk factor for developing glaucoma. It is measured with a Applanation Tonometer after instilling numbing drops in your eye. This is the most accurate, gold standard way to measure eye pressure.
Eye pressure is the most important risk factor for developing glaucoma. It is measured with a Applanation Tonometer after instilling numbing drops in your eye. This is the most accurate, gold standard way to measure eye pressure.
Statistically, normal eye pressures range from 8 to 21. However, normal eye pressure does NOT exclude glaucoma, and high eye pressure does NOT always mean you have glaucoma. If only it were that simple…
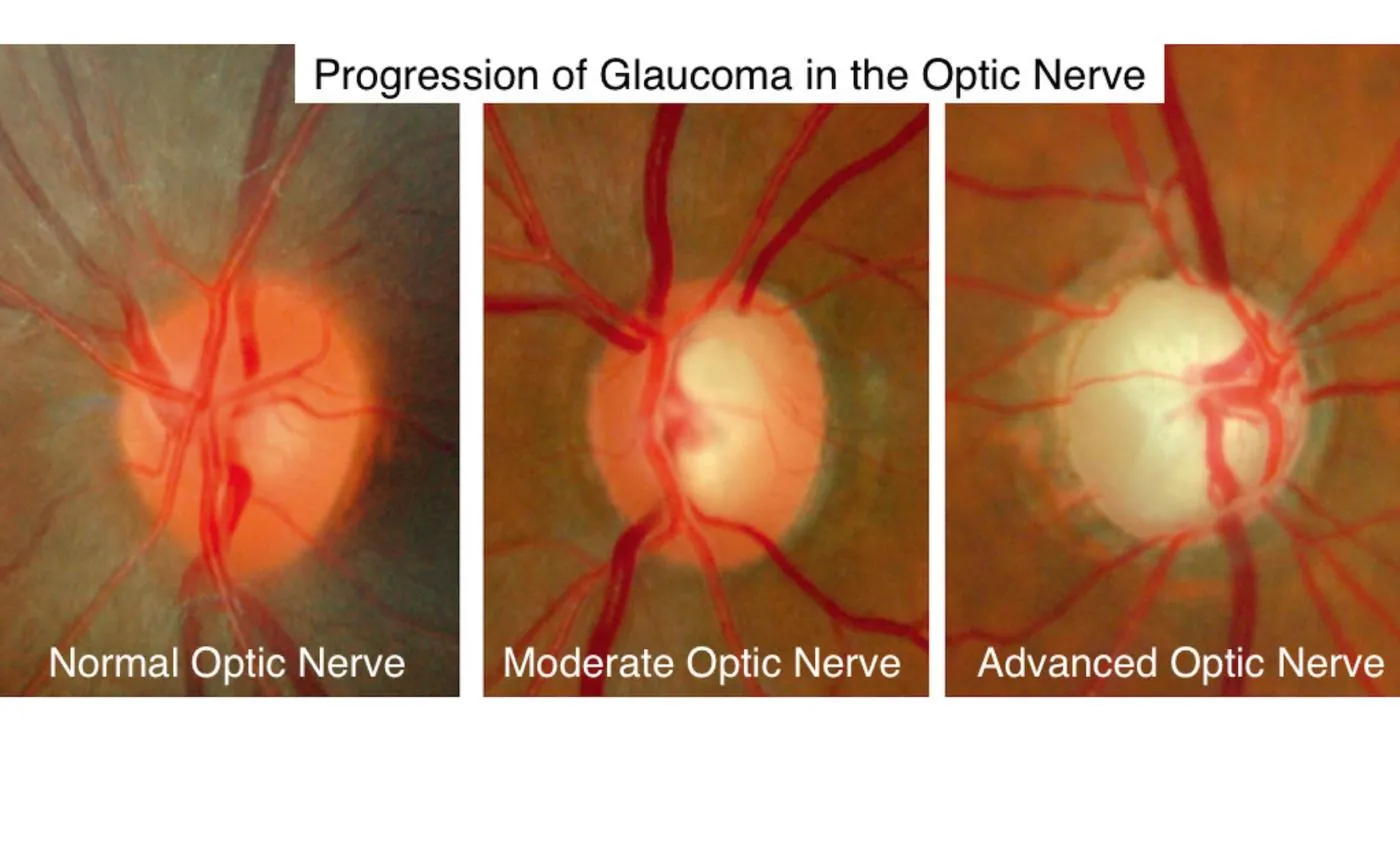 Dr. Thayer will examine the appearance of your optic nerve, looking for loss of nerve fiber and enlargement of the central area of the nerve. The picture shown to the left shows a normal nerve on the left, with a healthy orange rim of nerve fibers and a very small cup. The “cup” is the central area of the nerve that is not filled by nerve fibers. On the right, is an example of advanced glaucoma, with severe loss of rim nerve fibers and a greatly enlarged cup.
Dr. Thayer will examine the appearance of your optic nerve, looking for loss of nerve fiber and enlargement of the central area of the nerve. The picture shown to the left shows a normal nerve on the left, with a healthy orange rim of nerve fibers and a very small cup. The “cup” is the central area of the nerve that is not filled by nerve fibers. On the right, is an example of advanced glaucoma, with severe loss of rim nerve fibers and a greatly enlarged cup.
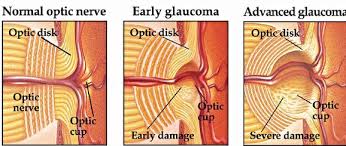
The picture shown shows this same process of progressive nerve fiber loss from a side view.
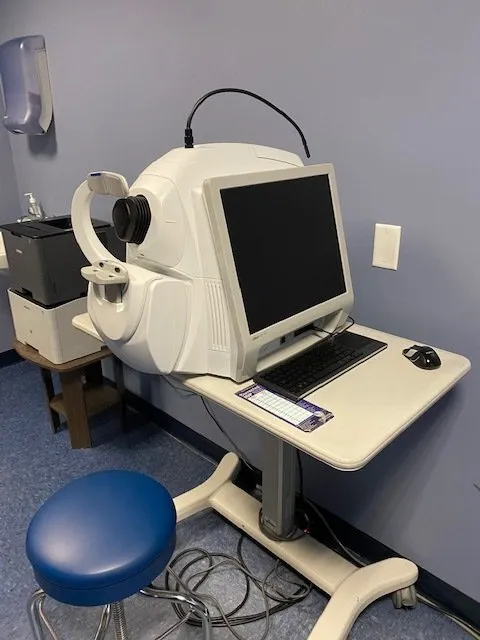 This is a technique for objectively measuring the thickness of nerve fibers going to the optic nerve. If you have, or are suspected of having, glaucoma, Dr. Thayer will image your nerve with this device. These images will then be repeated periodically, looking for any deterioration or loss of nerve fiber thickness.
This is a technique for objectively measuring the thickness of nerve fibers going to the optic nerve. If you have, or are suspected of having, glaucoma, Dr. Thayer will image your nerve with this device. These images will then be repeated periodically, looking for any deterioration or loss of nerve fiber thickness.
The picture shown below is an example of the information one can get with this technology. This is from a patient with advanced nerve fiber layer loss.
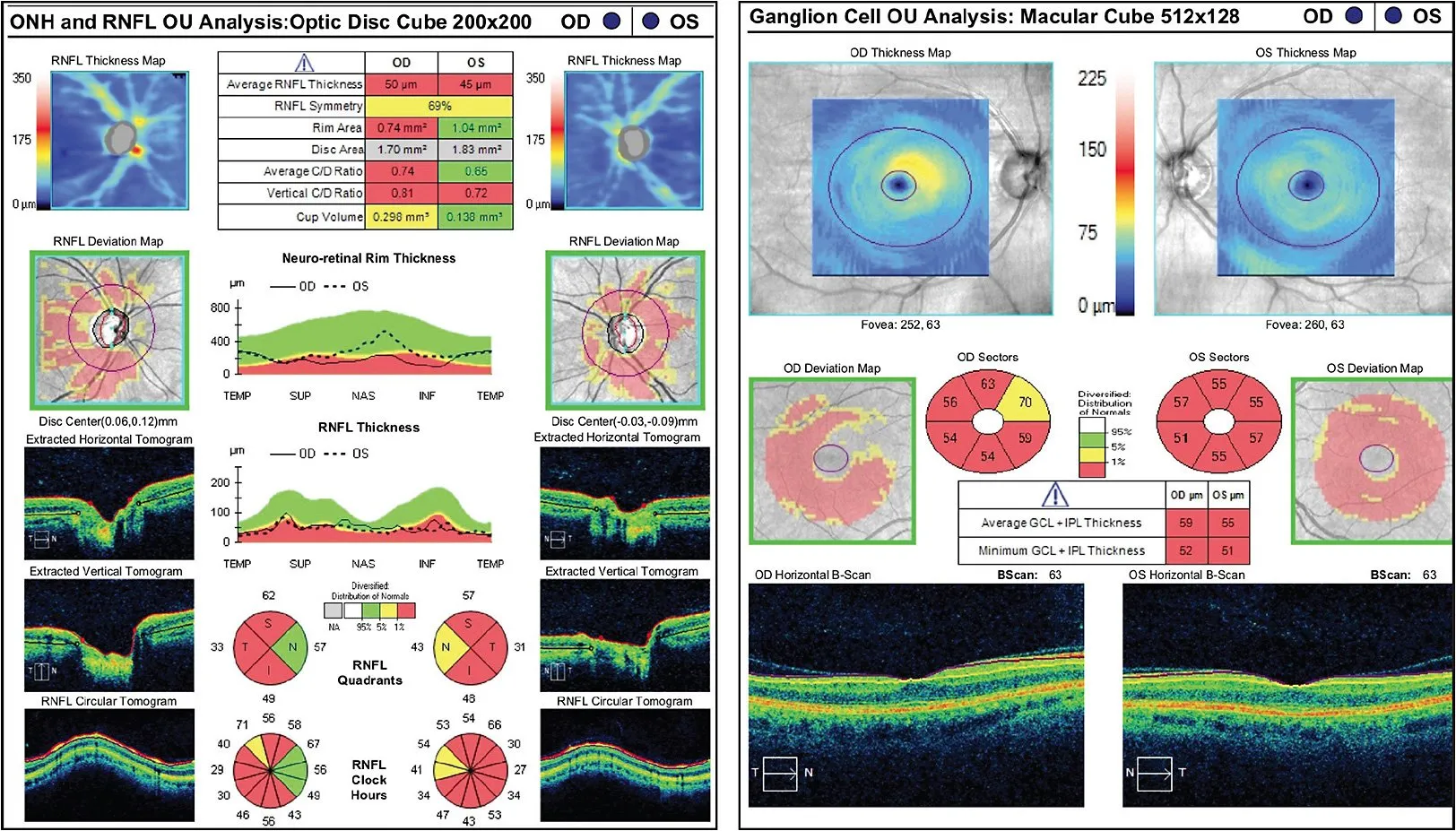
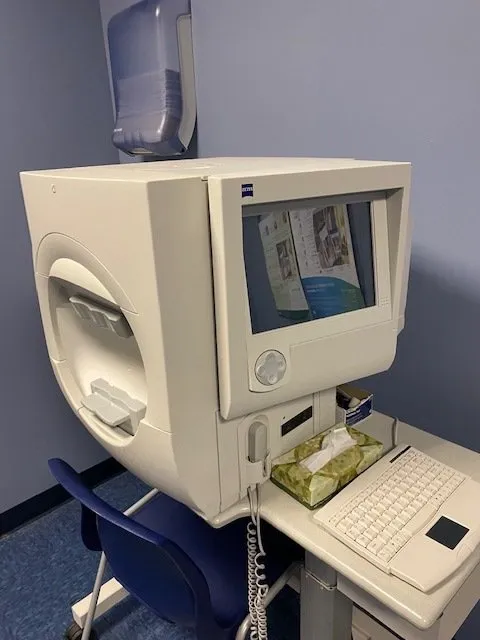 In glaucoma, the earliest vision loss occurs in the peripheral vision. The visual field analyzer is a subjective test in which the patient signals their ability, or inability, to see lights presented in their peripheral visual field. The test takes about five minutes per eye.
In glaucoma, the earliest vision loss occurs in the peripheral vision. The visual field analyzer is a subjective test in which the patient signals their ability, or inability, to see lights presented in their peripheral visual field. The test takes about five minutes per eye.
 The thickness of your cornea can affect the accuracy of eye pressure measurements, so it will be measured and a correction factor may be applied to your measured eye pressure. Studies have shown that thin corneas are associated with an underestimation of eye pressure and an increased risk of glaucoma.
The thickness of your cornea can affect the accuracy of eye pressure measurements, so it will be measured and a correction factor may be applied to your measured eye pressure. Studies have shown that thin corneas are associated with an underestimation of eye pressure and an increased risk of glaucoma.
 This is a method of examining the drainage angle of the eye that helps Dr. Thayer differentiate between open and closed angle glaucoma, as well as determine suitabilty for various glaucoma treatments. It involves numbing the eye with a drop, and placing a contact lens with a mirror on the front of the eye.
This is a method of examining the drainage angle of the eye that helps Dr. Thayer differentiate between open and closed angle glaucoma, as well as determine suitabilty for various glaucoma treatments. It involves numbing the eye with a drop, and placing a contact lens with a mirror on the front of the eye.

An example of what can be seen with gonioscopy.
Treating Glaucoma
options for treatment
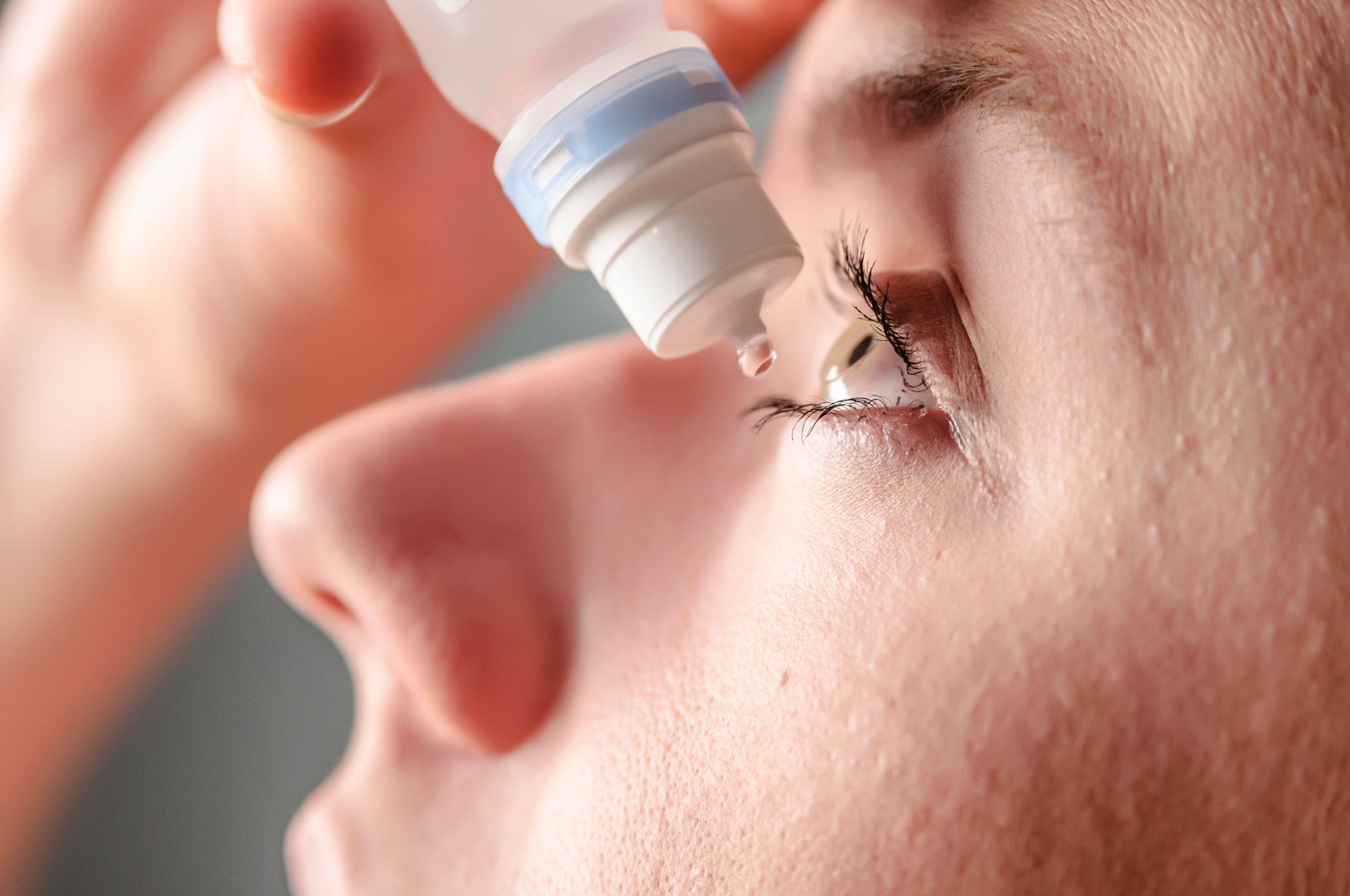
If you do receive a diagnosis of glaucoma, you will need treatment. That treatment will depend on the type of glaucoma you have, as well as its severity. In general, these are the categories of glaucoma treatment available.
- Laser
- SLT for Open Angle Glaucoma
- Iridotomy for Narrow Angles
- Medications
- Minimally Invasive Glaucoma Surgery (MIGS)
- Filtering Surgery and Valves
In the past, the first line of treatment was medications. However, with improvements in laser technology, the laser has become most ophthalmologists first line. It has many advantages compared to medications, and is universally covered by insurance. Dr. Thayer has the most modern lasers to perform these treatments in the office.
treatment options include
 For open angle glaucoma, SLT is clearly Dr. Thayer’s go-to option. It works about 80% of the time, it has minimal side effects, it takes two minutes, it usually lasts two to five years, it is covered by insurance, and it is repeatable. Even better, it avoids the expense, side effects, administration difficulties, and lack of compliance associated with eye drops. The machine to perform SLT is shown to the left in our clinic.
For open angle glaucoma, SLT is clearly Dr. Thayer’s go-to option. It works about 80% of the time, it has minimal side effects, it takes two minutes, it usually lasts two to five years, it is covered by insurance, and it is repeatable. Even better, it avoids the expense, side effects, administration difficulties, and lack of compliance associated with eye drops. The machine to perform SLT is shown to the left in our clinic.
Below is a video of a SLT being performed by a doctor in Australia, using a different brand of laser. The concept is the same.
 Iridotomy is a method of relieving a blockage of the drainage angle in patients with narrow angle glaucoma. It involves using a laser to punch a very small hole in the iris, thus allowing fluid within the eye to get to the structure through which it drains. This technique does not necessarily lower eye pressure, but it can prevent catastrophic, blinding increases in eye pressure that can be associated with an attack of angle closure glaucoma. It is also performed in the office and takes a few seconds to do.
Iridotomy is a method of relieving a blockage of the drainage angle in patients with narrow angle glaucoma. It involves using a laser to punch a very small hole in the iris, thus allowing fluid within the eye to get to the structure through which it drains. This technique does not necessarily lower eye pressure, but it can prevent catastrophic, blinding increases in eye pressure that can be associated with an attack of angle closure glaucoma. It is also performed in the office and takes a few seconds to do.
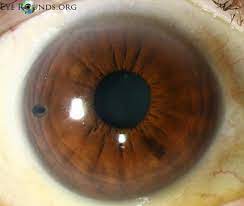 An example of an iris with an iridotomy is shown here. The iridotomy can be seen at 9 o’clock.
An example of an iris with an iridotomy is shown here. The iridotomy can be seen at 9 o’clock.
Also provided is a video explaining more about this procedure from the American Academy of Ophthalmology.
 In Dr. Thayer’s practice, medications are usually a second option if laser alone does not achieve an adequate reduction in eye pressure. There are at least six classes of medications, all with different dosing regimens and side effect profiles. A full discussion here is beyond the scope of this website.
In Dr. Thayer’s practice, medications are usually a second option if laser alone does not achieve an adequate reduction in eye pressure. There are at least six classes of medications, all with different dosing regimens and side effect profiles. A full discussion here is beyond the scope of this website.
Medications continue to perform a vital role in IOP management, especially in advanced glaucoma.
Unfortunately, medications have their disadvantages, to include cost, lack of adherence to dosing schedules, difficulty in self-administering the drops, and systemic and aesthetic side-effects.
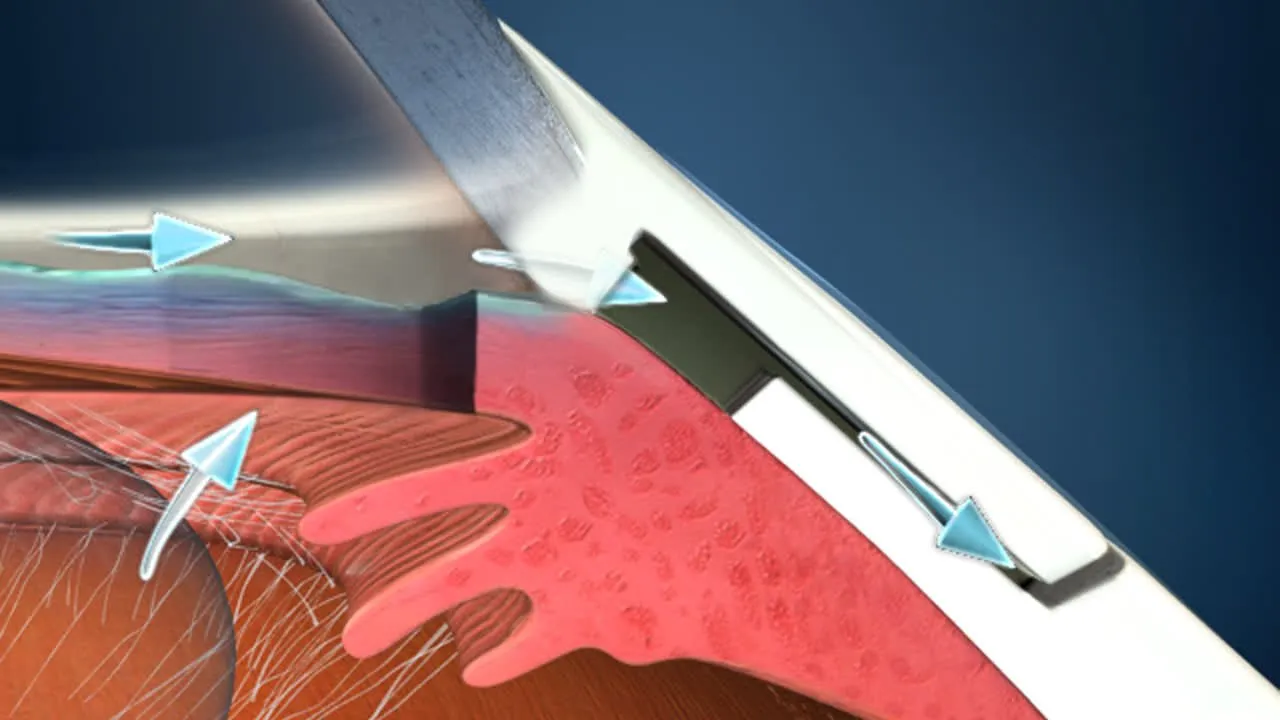
 This class of procedures generally refers to adjunctive drainage implants that can be placed at the time of cataract surgery. These can add to eye pressure control, reduce medication burden, and have less complications than the more invasive filtering surgery and valves. The example shown is of a Hydrus implant, placed at the time of cataract surgery. 77% of Hydrus Microstent patients saw a significant reduction in eye pressure, and 78% of all patients with a Hydrus Microstent were drop free at 2 years. This makes the Hydrus the best performing MIGS available to date.
This class of procedures generally refers to adjunctive drainage implants that can be placed at the time of cataract surgery. These can add to eye pressure control, reduce medication burden, and have less complications than the more invasive filtering surgery and valves. The example shown is of a Hydrus implant, placed at the time of cataract surgery. 77% of Hydrus Microstent patients saw a significant reduction in eye pressure, and 78% of all patients with a Hydrus Microstent were drop free at 2 years. This makes the Hydrus the best performing MIGS available to date.
More info on the Hydrus can be found here.
 When treatment with eye drops, pills, or laser surgery does not lower intraocular pressure to a safe level, Dr. Thayer may determine that glaucoma surgery should be performed. One way to reduce pressure in an eye with glaucoma is to make a new drain in the eye. This type of surgery is called a trabeculectomy. The other is to implant a tube drainage device. These procedures are reserved for advanced glaucoma.
When treatment with eye drops, pills, or laser surgery does not lower intraocular pressure to a safe level, Dr. Thayer may determine that glaucoma surgery should be performed. One way to reduce pressure in an eye with glaucoma is to make a new drain in the eye. This type of surgery is called a trabeculectomy. The other is to implant a tube drainage device. These procedures are reserved for advanced glaucoma.
Visit us today for your glaucoma treatment!
Your eye health is our top priority. From diagnosis to treatment our office provides you with the highest excellence in care. Contact us today to schedule your appointment with Dr. Thayer and discover the Thayer Difference.